Maternal Health: Outcomes Worsened and Disparities Persisted During the Pandemic
Fast Facts
Hundreds of women in the U.S. die each year from complications related to pregnancy and childbirth. Pregnant women with COVID-19 are more likely to experience complications.
We analyzed CDC data and found:
- Maternal deaths increased during the pandemic compared to 2018 and 2019
- COVID-19 contributed to 25% of maternal deaths in 2020 and 2021
- The maternal death rate for Black or African-American women was disproportionally higher compared to White and Hispanic or Latina women
Health and Human Services officials and stakeholders we interviewed said the pandemic worsened factors contributing to maternal health disparities, like access to care.

This page has been updated with a new photo that accurately reflects medical procedures.
Highlights
What GAO Found
Each year in the U.S., hundreds of women die from complications related to pregnancy and childbirth—known as maternal death. GAO's analysis of Centers for Disease Control and Prevention (CDC) data shows that maternal deaths increased during the COVID-19 pandemic. Further, the data show that COVID-19 was a contributing factor in one quarter of all maternal deaths in 2020 and 2021 combined.
Maternal Deaths, 2018 through 2021
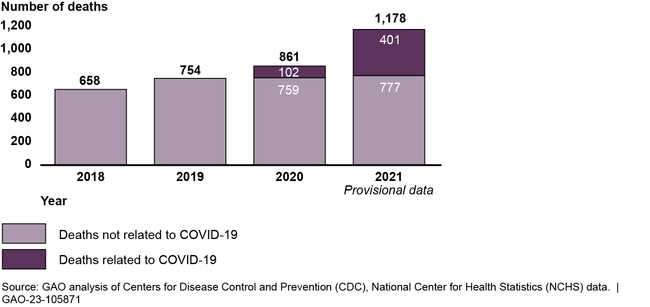
CDC data also show racial and ethnic disparities in the rate of maternal deaths per 100,000 live births per year. For example:
- The maternal death rate for Black or African-American (not Hispanic or Latina) women was 44.0 per 100,000 live births in 2019, then increased to 55.3 in 2020, and 68.9 in 2021. In contrast, White (not Hispanic or Latina) women had death rates of 17.9, 19.1, and 26.1, respectively.
- The maternal death rate for Hispanic or Latina women was lower (12.6) compared with White (not Hispanic or Latina) women (17.9) in 2019, but increased significantly during the pandemic in 2020 (18.2) and 2021 (27.5).
Disparities in other adverse outcomes, such as preterm and low birthweight births, persisted for Black or African-American (not Hispanic or Latina) women, according to GAO analysis of CDC data.
Stakeholders and Department of Health and Human Services (HHS) officials told GAO that the pandemic exacerbated the effects of social determinants of health—factors such as access to care, transportation, or technology; living environment; and employment—on maternal health disparities. For example, service reductions in public transportation and child care worsened existing barriers to accessing care. In addition, stakeholders and officials said the pandemic highlighted the effect racism has on maternal health. For example, physiological changes caused by chronic stress can increase the risk of maternal death, as well as severe illness from COVID-19.
Why GAO Did This Study
The COVID-19 pandemic presented challenges for maternal health, as pregnant women with COVID-19 are more likely to experience pregnancy complications, severe illness, or death. Research also shows racial and ethnic disparities in maternal deaths. For example, Black or African-American (not Hispanic or Latina) women experienced maternal death at a rate 2.5 times higher than White (not Hispanic or Latina) women in 2018 and 2019.
The CARES Act includes a provision for GAO to report on its COVID-19 pandemic oversight efforts. GAO also was asked to review how the pandemic has affected maternal health. This report describes, among other things, what available data show about maternal health outcomes and disparities during the pandemic.
To do this work, GAO analyzed the most recently available CDC data, including data from the National Vital Statistics System, to identify trends in maternal deaths and other outcomes, such as preterm births, by race and ethnicity. In addition, GAO reviewed agency documents and selected research; and interviewed officials at relevant HHS agencies, as well as eight stakeholders—including researchers, advocacy groups, and professional organizations—who were selected based on referrals from HHS agency officials and reviews of published research.
For more information, contact Carolyn L. Yocom at (202) 512-7114 or YocomC@gao.gov.
