COVID-19 in Nursing Homes: Outbreak Duration Averaged 4 Weeks and Was Strongly Associated with Community Spread
Fast Facts
From June 2020 through December 2021, nursing homes faced many separate COVID-19 outbreaks, with the average outbreak lasting 4 weeks.
We found that certain factors increased the likelihood that a nursing home would have a longer outbreak.
Specifically, transmission of COVID-19 in the community surrounding a nursing home had the strongest association, with nursing homes located in areas with high transmission more likely to have longer outbreaks. Longer COVID-19 outbreaks were also associated with nursing homes that were larger than 100 beds, experiencing reported staff shortages, and government-owned.
Highlights
What GAO Found
GAO analysis of data from the Centers for Disease Control and Prevention (CDC) shows that, from June 2020 through December 2021, nursing homes faced many separate COVID-19 outbreaks, with the average outbreak lasting 4 weeks. Officials GAO interviewed at six selected nursing homes in four states described a range of outbreak experiences, including critical challenges and some successes. For example, two critical challenges included:
- Staff shortages. Officials from five nursing homes described experiencing staffing shortages during outbreaks. For example, officials from one nursing home described a staffing crisis, noting that at one point the home was down about 25 percent of its workforce.
- Low staff morale. Officials from three nursing homes discussed the psychosocial effect the pandemic had on their staff and the difficulties in maintaining staff morale. For example, officials from one nursing home described how the outbreaks took away the joy of caregiving from staff, and officials believed that many staff were left traumatized.
GAO's analysis of CDC and Centers for Medicare & Medicaid Services (CMS) data found that transmission of COVID-19 in the community surrounding a nursing home, known as community spread, had the strongest association with the duration of an outbreak. Controlling for other factors, prior to the introduction of COVID-19 vaccines, nursing homes in counties experiencing low community spread had outbreaks that ended an estimated 7 days earlier than nursing homes in counties experiencing high community spread. GAO also found that most outbreaks (75 percent) began with a reported staff case during the first week. These results could indicate that, during times of higher community spread, staff have a greater likelihood of being exposed to the virus in the community and bringing it into the nursing home. Other factors GAO found that had a strong association with outbreak duration included nursing home size, reported staff shortages, and ownership type.
GAO Estimated COVID-19 Outbreak Duration for Nursing Homes with Selected Characteristics
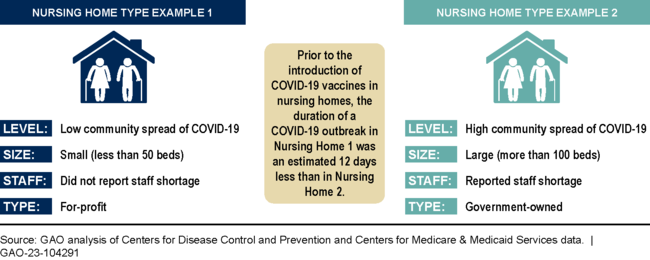

Note: Using multivariate statistical models, GAO estimated the association of nursing home factors, such as facility characteristics, with the likelihood that an ongoing COVID-19 outbreak would end during a given week.
Why GAO Did This Study
The COVID-19 pandemic has had a disproportionate effect on the more than 1 million residents in the nation's nursing homes. The initial unknown nature of the virus and the scope of the pandemic created unprecedented challenges. The Department of Health and Human Services, primarily through CMS and CDC, is responsible for taking steps to address COVID-19 in nursing homes, such as issuing relevant requirements and guidance.
Many studies have explored the factors associated with the presence or severity of COVID-19 in nursing homes. However, little was known about the factors associated with the duration of COVID-19 outbreaks within nursing homes.
The CARES Act directs GAO to monitor the federal pandemic response. GAO was also asked to review CMS oversight of nursing homes in light of the pandemic. This report examines how COVID-19 outbreaks affected nursing homes, and determines how nursing home factors were associated with outbreak duration.
GAO analyzed CDC and CMS nursing home data from June 2020 through December 2021, in a statistical model, and conducted a literature review. GAO also interviewed representatives from nursing homes and state agencies from a non-generalizable sample of four states. The states were selected for variation in factors such as number of nursing home beds and COVID-19 cases.
For more information, contact John Dicken at (202) 512-7114 or dickenj@gao.gov.
